A team of researchers and physicians led by Professor Ron Alterovitz from UNC’s department of computer science has demonstrated, for the first time, a robotic needle capable of autonomously maneuvering through intricate lung tissue while avoiding obstacles and important lung structures.
 While self-driving cars zoom through the streets of San Francisco, medical robots may soon be zooming through the body – autonomously steering around anatomical obstacles to reach important medical targets. Just as it is difficult for self-driving cars to recognize and avoid obstacles such as pedestrians in real-time, it is challenging for physicians or medical robots to navigate through complicated anatomy, avoid significant anatomical obstacles such as nerves and blood vessels, and safely and accurately reach a target (such as a tumor).
While self-driving cars zoom through the streets of San Francisco, medical robots may soon be zooming through the body – autonomously steering around anatomical obstacles to reach important medical targets. Just as it is difficult for self-driving cars to recognize and avoid obstacles such as pedestrians in real-time, it is challenging for physicians or medical robots to navigate through complicated anatomy, avoid significant anatomical obstacles such as nerves and blood vessels, and safely and accurately reach a target (such as a tumor).
A team of researchers and physicians led by Professor Ron Alterovitz from the University of North Carolina at Chapel Hill have demonstrated, for the first time, a robotic steerable needle capable of autonomously maneuvering through living tissue to reach a target while avoiding anatomical obstacles. The team published this milestone result in the journal Science Robotics, the most prestigious journal covering robotics research.
“Commercial medical robots sold today are typically teleoperated, meaning a human is always directly controlling every motion,” said Professor Alterovitz. “By leveraging the power of robotics and AI, we developed a robot capable of autonomously steering needles to targets in living tissue with unprecedented accuracy and safety.”
During complicated medical procedures, if a medical instrument is off by even a few millimeters, the results can be disastrous. For example, a failure to precisely reach a suspicious nodule in the lung for biopsy can result in an inaccurate diagnosis, allowing cancer to spread untreated. An autonomous medical robotic needle could be used to facilitate safer, more accurate procedures throughout the body including biopsies, directed drug delivery, and localized radiation cancer treatment. Needles are a fundamental tool for such procedures because they are minimally invasive which reduces the patient’s pain and recovery time.

Developing the autonomous robotic steerable needle is a multi-disciplinary effort by computer scientists, engineers, and physicians. The team at the University of North Carolina at Chapel Hill (UNC) includes the project’s Principal Investigator, Ron Alteorvitz, PhD, from the Department of Computer Science, and includes physicians from the UNC School of Medicine, Jason Akulian, MD, MPH, with expertise in interventional pulmonology, and Yueh Z. Lee, MD, PhD, with expertise in radiology. The team also includes engineering expertise from the group of Robert J. Webster III, PhD, at Vanderbilt University and Alan Kuntz, PhD, a former graduate student at UNC who is now faculty at the University of Utah.
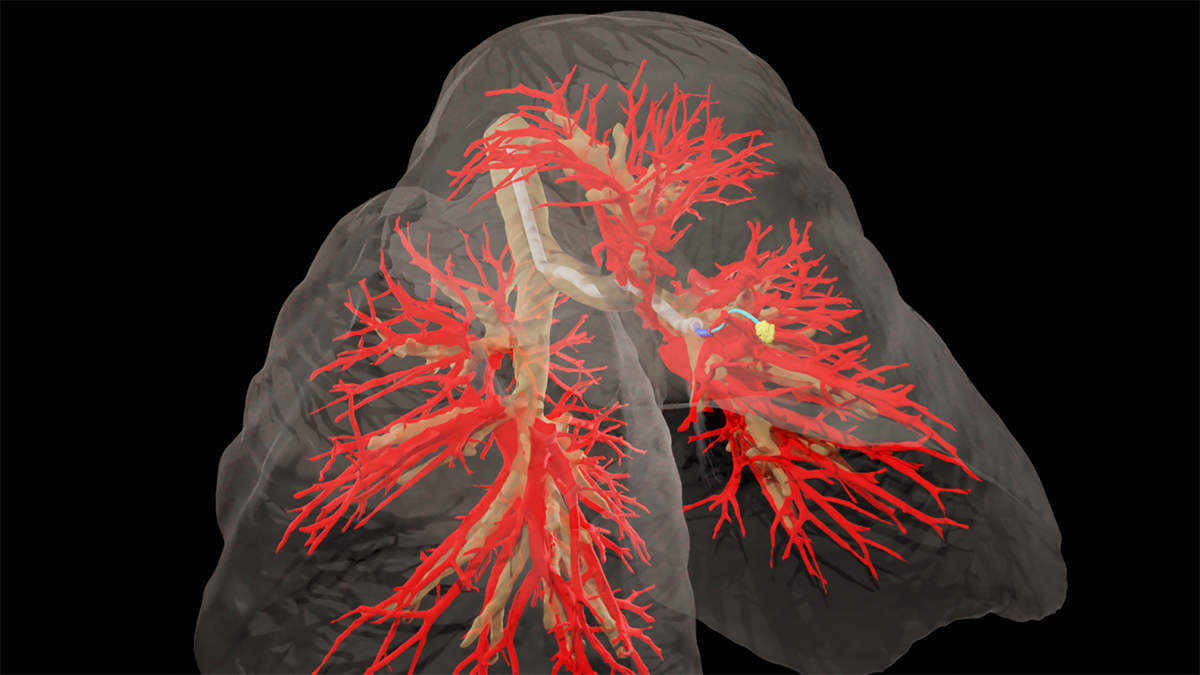
The research team successfully demonstrated this novel robot in one of the most challenging organs: the breathing lung. Lung cancer is the leading cause of cancer-related deaths in the United States. Some tumors are extremely small and hide deep within lung tissue, making it difficult for surgeons to reach them. Unlike other organs, the lungs are constantly expanding and contracting in the chest cavity. Reaching a target in the lung is like asking a self-driving car to parallel park with millimeter precision while the road is deforming under its wheels. This can make targeting especially difficult in a living, breathing subject. According to Dr. Akulian, it’s like shooting at a moving target.
“This technology allows us to reach targets we can’t otherwise reach with a standard or even robotic bronchoscope,” said Dr. Akulian, co-author on the paper.
The robot is made of several separate components. A mechanical control provides controlled thrust of the needle to go forward and backward and the needle design allows for steering along curved paths. The needle is made from a nickel-titanium alloy and has been laser etched to increase its flexibility, allowing it to move effortlessly through tissue. As it moves forward, the etching on the needle allows it to steer around obstacles with ease. Other attachments, such as catheters, could be used together with the needle to perform procedures such as lung biopsies.
To drive through tissue, the needle needs to know where it is going. The research team used CT scans of the subject’s thoracic cavity to create three-dimensional models of the lung, including the airways, blood vessels, and the chosen target. Using this 3-D model and once the needle has been positioned for launch, their AI-driven software instructs it to automatically travel from “Point A” to “Point B” while avoiding important structures.
“The autonomous steerable needle we’ve developed is highly compact, but the system is packed with a suite of technologies that allow the needle to navigate autonomously in real-time,” said Professor Alterovitz. “It’s akin to a self-driving car, but it navigates through lung tissue, avoiding obstacles like significant blood vessels as it travels to its destination.”
The team plans to continue to work to bring robotic steerable needles closer to clinical use in humans by refining the system and providing further guarantees on performance in challenging cases, while also exploring new applications. “While there’s still a lot of work to be done, I’m very excited about continuing to push the boundaries of what we can do for patients,” said Dr. Akulian. Professor Alterovitz added, “We plan to continue creating new autonomous medical robots that combine the strengths of robotics and AI to improve medical outcomes for patients facing a variety of health challenges while providing guarantees on patient safety.”
The research paper is available online in the journal Science Robotics.
Courtesy of the department of computer science
